Astigmatism is one of the most common refractive conditions, yet many patients don’t fully understand what it is or how it affects their vision. Because symptoms can be subtle or inconsistent, patients may normalize visual discomfort rather than seek answers. By offering clear, easy-to-understand guidance, you can help patients recognize astigmatism, understand its impact, and feel confident in choosing solutions that better support their daily visual needs.
Understanding the Astigmatic Patient
Astigmatic patients include both adults and children who experience blurred or distorted vision at multiple distances. Many already wear glasses or contact lenses but still report visual discomfort or fatigue. Their daily routines often involve extended near work, such as reading, using computers, or engaging with digital devices. Driving can also be challenging, particularly at night, when glare and distortion become more noticeable.
Active individuals may face additional difficulties with distance clarity during sports or outdoor activities. Addressing these visual needs is crucial: proper correction can reduce eye strain, headaches, and fatigue, while enhancing overall quality of life and confidence in visual performance.
What Patients Should Know About Astigmatism
Astigmatism occurs when the eye’s curvature is irregular, preventing light from focusing evenly on the retina. Mild astigmatism may produce little to no noticeable symptoms, but higher levels can cause objects to appear blurred, stretched, or distorted. Many patients with more moderate astigmatism may not realize why they experience headaches, eye strain, or difficulty seeing clearly—especially at night or when using digital devices. Discussing these signs with your patients can help you guide them toward solutions that improve their comfort and clarity.
Patients with astigmatism may report:
- Blurred or distorted vision at distance or near
- Difficulty with night vision, such as blurred headlights
- Squinting to achieve clarity
- Shadowed or doubled images of bright objects (e.g., the moon or stars)
- Eye strain or headaches during prolonged visual tasks
- Trouble distinguishing similar letters or numbers (e.g., “V” vs. “W,” “3” vs. “8”)
- Challenges reading digital screens, recognizing traffic signs, or seeing clock hands
Clearer Vision, Realistic Expectations: How to Explain Solutions for Astigmatism
When discussing solutions, it’s important to set realistic expectations. Astigmatism has no absolute “cure,” and some visual distortion may remain. However, modern lens technology can significantly improve clarity and comfort.
Single vision lenses: MySV® single vision lenses with 360° Visual Comfort™ provide effective correction for astigmatism, whether the patient is nearsighted or farsighted.
Progressive lenses: iD LifeStyle® 4 and iD MyStyle® 3 lenses with Binocular Harmonization Technology help balance visual performance between both eyes—especially useful when prescriptions differ, which is common in astigmatic patients.
For astigmatic patients, prescribing a quality free form lens design can make a meaningful difference in visual clarity and comfort by more precisely correcting their prescription. That benefit depends on clear communication during the hand-off from the ECP to the optician. When the ECP clearly states, “This patient is astigmatic and I prescribed a free form lens design to specifically help in correcting it,” it helps ensure the prescription intent is preserved. Stepping down to a conventional lens design—especially for single-vision wearers—can be detrimental and may compromise the visual outcome intended for the patient.
For most patients with regular astigmatism, spectacles with properly designed lenses such as these options from HOYA can provide clear, comfortable vision. However, in cases of irregular astigmatism, where the corneal surface is uneven, standard spectacle lenses may not fully correct visual distortion. In these situations, hard contact lenses can help create a smoother optical surface, allowing light to focus more evenly on the retina and improving visual clarity. For more information and visual references you can share with your patients, see this resource.
Talking Points for Patient Conversations
When discussing astigmatism, use open-ended questions that encourage patients to describe their visual experiences in their own words. This helps uncover concerns they may not immediately associate with astigmatism and keeps the conversation patient-centered.
Examples of open-ended questions include:
- “How do your eyes feel at the end of the day or when driving at night?”
- “Can you describe situations where your vision feels less clear or less comfortable?”
- “What do you notice about your vision when reading or using digital devices?”
- “How does your vision feel in different lighting conditions, such as bright daylight or low light?”
- “Are there any activities where you feel your vision affects your comfort or confidence?”
These questions allow patients to share experiences related to clarity, comfort, and visual performance without suggesting a diagnosis, creating a natural opportunity to explain astigmatism and appropriate HOYA® lens solutions.
You can also reinforce explanations with visual tools, such as Figure 1 below, or in-office displays to help patients see how astigmatism affects vision and how lens designs can help.
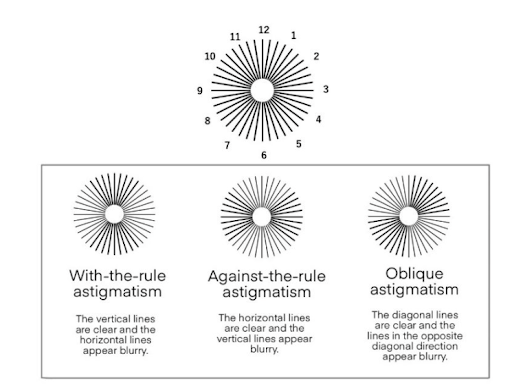
Figure 1
Helping patients understand their astigmatism empowers them to take an active role in their eye care. With clear explanations, realistic expectations, and tailored HOYA® solutions, ECPs can provide reassurance and meaningful improvements in visual comfort and performance—giving patients the confidence they need to see their world more clearly.
